“Waiting for the right information isn’t hesitation , it’s precision.”
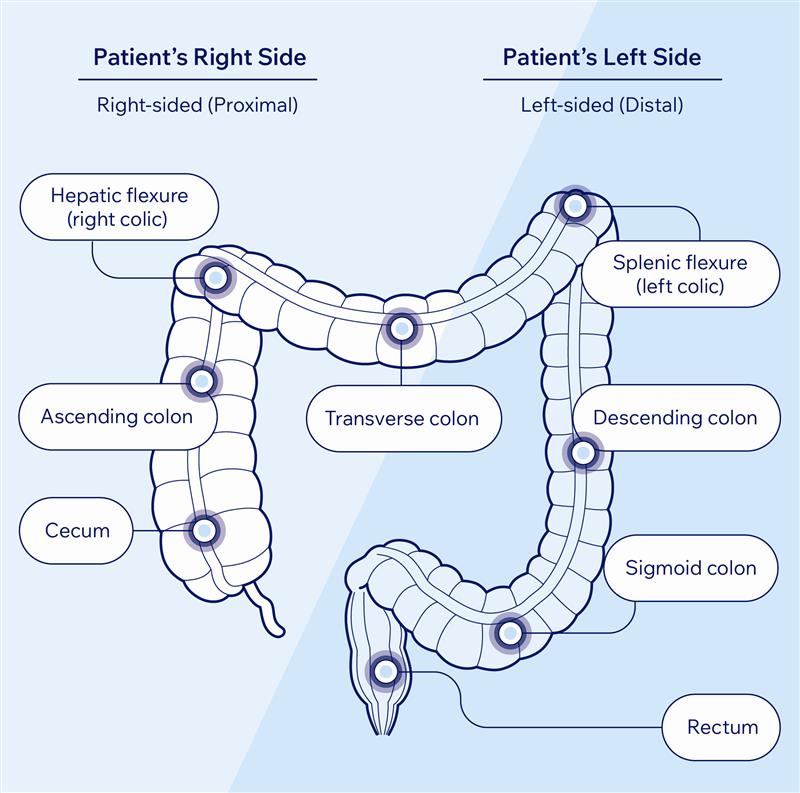
Biomarkers are pieces of information about your health. For colorectal cancer, relevant biomarkers include the location of a tumor, substances released by the tumor that circulate in the blood, changes in the genes or proteins of your tumor cells, or genetic changes in you.
The results of biomarker testing provide you and your care team with critical information about you and your cancer that is used in making various treatment decisions. Colorectal cancers are not all the same; each cancer has characteristics that influence how it should be treated, and you and your healthcare team will make treatment decisions together.
Nearly half of the oncology drugs approved in the U.S. since 1998 are precision therapies that rely on biomarker testing. Here are the five key areas where your results change what happens next.
What it is
Targeted therapy is cancer treatment that uses medications to target cancer cells directly and more precisely destroy cancer. Nearly half of the oncology drugs approved in the U.S. since 1998 are precision therapies that rely on biomarker testing.
Why it matters
All of these ways of targeting cancer cells depend on information about your cancer’s biomarkers. Biomarkers help your care team understand the specific type of colorectal cancer you have so they can match you with the most effective treatment. Tumors that have microsatellite instability, a biomarker also called MSI-High or dMMR, often respond well to immunotherapy. Biomarkers can also reveal whether your tumor is likely to respond to certain therapies or if alternative approaches may be needed. In colorectal cancer with BRAF V600E mutation, BRAF inhibitors can be combined with EGFR inhibitors and MEK inhibitors to reduce the likelihood of drug resistance. By identifying these unique characteristics early, your team can build a more personalized and effective treatment plan.
What it is
Decision-making about cancer treatment involves not only choosing the right treatments but also avoiding the wrong ones. There are treatments that may be ineffective against a particular colorectal cancer. And certain treatments may actually be especially harmful or dangerous in certain people.
Why it matters
Using a treatment that isn’t effective for your type of cancer can delay you from getting the care that could actually help. This lost time may allow the cancer to grow or become harder to treat. It also means you’re exposed to side effects from a therapy that isn’t providing real benefit. Your biomarkers can provide clues about which treatments won’t be effective. For example, EGFR inhibitors are not usually effective in patients with KRAS mutations, so they aren’t given.
Some biomarkers, like DPD/DPYD and UGT1A1, can also predict which treatments may be particularly harmful to you. Chemotherapy drugs usually have some negative side effects, but in some people, they are severe or even fatal. Drug metabolism is a process your body uses to break down medicine into forms that are easier for your body to use or get rid of. Enzymes are chemicals in the body that help this process. In people who have drug metabolism enzymes that are abnormal or absent, the severity of side effects can increase. Knowing about your drug metabolism enzymes through biomarker testing can help your doctor choose the right dose of medicine for you or even avoid certain drugs that would be dangerous to you.
What it is
Prognosis is the expected course of a disease. Some biomarkers can predict the outlook of your cancer, including how aggressive it will be. Biomarkers may also give information about the risk of the cancer returning after treatment. This helps your care team decide what follow-up care you may need. It can also give you a better understanding of what to expect during and after treatment.
Why it matters
Prognostic information can affect how your cancer is treated. It guides decisions about whether or not to use chemotherapy after surgery, a treatment called adjuvant chemotherapy. Some patients with stage II colorectal cancer may be cured by surgery alone, but in patients with an aggressive subtype of colorectal cancer, adjuvant chemotherapy is recommended to kill any remaining cancer cells and prevent recurrence.
Prognosis also impacts choices about how and when to check to make sure the cancer hasn’t come back after treatment. After colorectal cancer treatment, patients and their healthcare teams make decisions about this follow-up care, including imaging scans, blood tests, and colonoscopies. If a patient has a colorectal cancer with biomarker results that predict a higher risk of recurrence, follow-up care will involve more frequent testing to look for any signs of the cancer returning.
What it is
There are times when a person who is at very high risk of cancer recurrence may have more extensive surgery for their colorectal cancer to lower the risk of their cancer coming back. There are also rare situations in which patients at very high risk of CRC may have surgery to prevent colorectal cancer before they ever get it, called prophylactic or preventive surgery. Biomarkers also play a role in determining the surgical approach to tumors that have spread outside the colon and rectum, called metastases.
Why it matters
The type of surgery a person has for colorectal cancer, or even for precancerous colorectal polyps, can be guided by biomarker testing results. Biomarker testing (including genetic testing) can reveal whether a patient has a hereditary cancer syndrome. Hereditary cancer syndromes are health conditions that are passed down in families through genes. People can be born with a change in their DNA that increases their risk of cancer. About 5% of colorectal cancers are due to a hereditary cancer syndrome.
The most common hereditary colorectal cancer syndrome is Lynch Syndrome. People with Lynch syndrome have a 40-80% lifetime risk of CRC, with women at the lower end of the range, and men at the higher end. Together with their healthcare teams, patients with colorectal cancer from Lynch Syndrome may decide to have more extensive surgical procedures, like having more of their colon removed and not just the segment affected by a tumor. This is because of the very high likelihood their cancer will come back. More extensive surgery can lower that risk. Familial Adenomatous Polyposis and its subtypes cause about 1% of colorectal cancers, but the lifetime risk of CRC in people with untreated FAP is close to 100%. Therefore, people with Familial Adenomatous Polyposis often have total removal of their colon and rectum, even if they are diagnosed in the precancerous stage. If precancerous tumors are left untreated, they will become cancer. And because of FAP, these patients will continue to develop precancerous tumors. Removal of the organs that develop the tumors greatly reduces the risk of colorectal cancer.Biomarkers can also be used in decision-making about surgery to remove tumors that have spread outside the colorectum, called metastases or metastatic tumors. Removal of metastases, or metastasectomy, may be made possible by targeted therapy, which is guided by biomarker testing. For example, tumors with microsatellite instability may shrink after a strong response to immunotherapy, making them resectable. In addition, a good response to targeted therapies in HER2 amplified tumors, tumors with NTRK fusion, or tumors with KRAS G12C mutation may make these metastases small removable. Other RAS mutations and BRAF V600E mutations often predict poor outcomes from aggressive surgery to remove liver metastases.
What it is
More than half of oncology clinical trials involve the use of biomarkers, and this number is on the rise. Around 55% of all oncology clinical trials in 2018 involved the use of biomarkers, as compared with about 15% in 2000.
Why it matters
In many of these trials, biomarkers are used for patient selection, either to include patients with certain biomarker testing results or to decide they are not a good candidate for the trial. In this case, biomarker testing serves as a matchmaker between patients and clinical trials.
An increasing number of clinical trials study patients with multiple tumor types that share a biomarker, for example, all solid tumors with NTRK fusion, which could include patients with colorectal cancer, lung cancer, or thyroid cancer. These are called basket trials, because patients with different diseases are considered as one “basket” of patients because they have the same biomarker. This is in contrast to trials that focus on one specific cancer, instead focusing on the shared biomarker. The only way to be matched with a trial like this is through biomarker testing.
Another type of clinical trial treats patients with a single cancer type, but patients are assigned to different treatments based on their distinct biomarkers. This is called an umbrella trial because it consists of smaller sub-trials under the umbrella of the larger trial. These designs greatly increase trial efficiency for targeted agents but depend on timely, accurate biomarker testing.
It’s important to have biomarker testing results before starting treatment, so that clinical trial matching can happen first. Many clinical trials require that patients be “treatment-naive” to participate. That means that patients who have started treatment already will be ineligible for those trials. Early biomarker testing and waiting for results gives patients the greatest chance to participate in a clinical trial.
These answers have been prepared by GCCA and are intended for educational purposes. They do not constitute medical advice. Always discuss your care with your healthcare team.
Biomarker testing (also called molecular testing) looks at your tumor genetic makeup to find specific changes that can guide treatment decisions. For colorectal cancer, guidelines from ESMO, ASCO, and NCCN recommend comprehensive biomarker testing for all patients with metastatic disease.
The short answer: yes, if you have been diagnosed with colorectal cancer, you should ask your oncologist about comprehensive biomarker testing before any treatment begins.
In most cases, the 1–3 weeks for biomarker results to return will not meaningfully change your outcome — but starting treatment without results can. Beginning the wrong chemotherapy regimen can cause serious harm and delay access to more effective targeted therapies.
There are rare situationssuch as a bowel obstruction where immediate intervention is necessary. But for many newly diagnosed patients, the wait is worth it.
Biomarker testing results are typically returned in about 1-3 weeks. In areas where samples must be shipped to specialized laboratories, results may take several weeks.
Ask your oncologist when to expect results, and ask for them to be expedited if possible. Some institutions offer reflex testingwhere comprehensive panels are automatically ordered at diagnosis, which can reduce delays.
It is not too late. Biomarker results are still valuable even if treatment has already started. They can inform whether to continue your current regimen, switch to a more targeted approach, or seek a second opinion.
Be aware that having started treatment may disqualify you from some clinical trials that require treatment-naive status.
A direct question works well: “Has comprehensive molecular biomarker testing been ordered for my tumor? Can we wait for those results before starting treatment?”
You can also ask: “Will my tumor be tested for KRAS, NRAS, BRAF, MSI/MMR status, HER2, and DPYD before we choose a treatment regimen?”
Download our free Questions to Ask Your Healthcare Team guide below. It includes these questions with space to write your results.
Downloadable from the Know Your Biomarker site.

Print-ready guide with questions about biomarker testing and space to write your answers. Bring extra copies, one for you, one for your caregiver.

What is a biomarker? How are they used in CRC? Who should have biomarker testing? Your questions answered in plain-language for patients and families.

Print-ready guide with the very basics of biomarkers and what they can mean for treatment.
Learn more on knowyourbiomarker.org
Found in ~10% of CRC cases; drives targeted therapy options.
The most commonly mutated gene in colorectal cancer.
Affects response to anti-EGFR therapies.
Key indicator for immunotherapy eligibility.
Emerging target with new treatment options in CRC.
Blood marker used to monitor treatment response and recurrence.
Circulating tumor DNA detected through liquid biopsy.
Genetic variant that can cause fatal chemotherapy toxicity.
Hereditary condition that significantly increases CRC risk.
Inherited polyposis syndromes requiring early intervention.